×
It looks like you're using an obsolete version of internet explorer. Internet explorer is no longer supported by Microsoft since the end of 2015. We invite you to use a newer browser such as Firefox, Google Chrome or Microsoft Edge.
40797 views
Program
| 12.30 | Introduction |
| 12.32 |
Overview of devices: ○ Veniti stent – Stephen Black ○ Wallstent – Olivier Hartung ○ IVUS – Peter Neglen |
| 12.47 |
Case in box n°1: May-Thurner syndrome Panel discussion |
| 12.57 |
Case in box n°2: May-Thurner syndrome Panel discussion |
| 13.07 |
Acute DVT: ○ Goals and history of clot removal strategies – Yves Alimi ○ PMT - Stephen Black |
| 13.25 |
Treatment of chronic lesions: ○ Recanalization – Olivier Hartung |
| 13.33 |
Case in box n°3: Left femoro iliac vein recanalization and stenting Panel discussion |
| 13.41 |
Case in box n°4: Left femoro iliac vein recanalization and stenting Panel discussion |
| 13.55 | Conclusion |
Educational objectives
- Diagnostic approach for patients with suspected ilio-femoral vein obstructions
-
Tips and Tricks for venous recanalization in patients with:
- Acute DVT
- May Thurner Syndrome
- Chronic obstructions of the ilio-femoral vein system
- Stent design, performance and available evidence
- Value of Intravascular ultrasound (IVUS) for venous recanalizsation
Audience
- Endovascular specialists (Vascular Surgeons, Interventional Radiologists, Angiologists and Interventional Cardiologists) interested and/or specialized in venous interventions
- Referring physicians of patients with venous disease
Shooting date : 2017-10-13
Last update : 2018-06-26
Last update : 2018-06-26
Join the Discussion
Suggestions
Tuesday, September 8th 2020 from 12:30pm to 02pm (GMT+2)
Honolulu : Tuesday, September 8th 2020 from 12:30am to 02am (GMT+2)
San Francisco : Tuesday, September 8th 2020 from 03:30am to 05am (GMT+2)
New York : Tuesday, September 8th 2020 from 06:30am to 08am (GMT+2)
Buenos Aires : Tuesday, September 8th 2020 from 07:30am to 09am (GMT+2)
Reykjavik : Tuesday, September 8th 2020 from 10:30am to 12pm (GMT+2)
London / Dublin : Tuesday, September 8th 2020 from 11:30am to 01pm (GMT+2)
Paris / Berlin : Tuesday, September 8th 2020 from 12:30pm to 02pm (GMT+2)
Istanbul : Tuesday, September 8th 2020 from 01:30pm to 03pm (GMT+2)
Moscou / Dubaï : Tuesday, September 8th 2020 from 02:30pm to 04pm (GMT+2)
Bangkok : Tuesday, September 8th 2020 from 05:30pm to 07pm (GMT+2)
Shanghai : Tuesday, September 8th 2020 from 06:30pm to 08pm (GMT+2)
Tokyo : Tuesday, September 8th 2020 from 07:30pm to 09pm (GMT+2)
Sydney : Tuesday, September 8th 2020 from 09:30pm to 11pm (GMT+2)
Wellington : Tuesday, September 8th 2020 from 11:30pm to 01am (GMT+2)
San Francisco : Tuesday, September 8th 2020 from 03:30am to 05am (GMT+2)
New York : Tuesday, September 8th 2020 from 06:30am to 08am (GMT+2)
Buenos Aires : Tuesday, September 8th 2020 from 07:30am to 09am (GMT+2)
Reykjavik : Tuesday, September 8th 2020 from 10:30am to 12pm (GMT+2)
London / Dublin : Tuesday, September 8th 2020 from 11:30am to 01pm (GMT+2)
Paris / Berlin : Tuesday, September 8th 2020 from 12:30pm to 02pm (GMT+2)
Istanbul : Tuesday, September 8th 2020 from 01:30pm to 03pm (GMT+2)
Moscou / Dubaï : Tuesday, September 8th 2020 from 02:30pm to 04pm (GMT+2)
Bangkok : Tuesday, September 8th 2020 from 05:30pm to 07pm (GMT+2)
Shanghai : Tuesday, September 8th 2020 from 06:30pm to 08pm (GMT+2)
Tokyo : Tuesday, September 8th 2020 from 07:30pm to 09pm (GMT+2)
Sydney : Tuesday, September 8th 2020 from 09:30pm to 11pm (GMT+2)
Wellington : Tuesday, September 8th 2020 from 11:30pm to 01am (GMT+2)
State-of-the-Art Endovascular Management of Venous Diseases
Embolization - Venous Stenting - Glue Ablation
Share
May 2014
Honolulu : Monday, April 7th 2014 from 04am to 05am (GMT+2)
San Francisco : Monday, April 7th 2014 from 07am to 08am (GMT+2)
New York : Monday, April 7th 2014 from 10am to 11am (GMT+2)
Buenos Aires : Monday, April 7th 2014 from 11am to 12pm (GMT+2)
Reykjavik : Monday, April 7th 2014 from 02pm to 03pm (GMT+2)
London / Dublin : Monday, April 7th 2014 from 03pm to 04pm (GMT+2)
Paris / Berlin : Monday, April 7th 2014 from 04pm to 05pm (GMT+2)
Istanbul : Monday, April 7th 2014 from 05pm to 06pm (GMT+2)
Moscou / Dubaï : Monday, April 7th 2014 from 06pm to 07pm (GMT+2)
Bangkok : Monday, April 7th 2014 from 09pm to 10pm (GMT+2)
Shanghai : Monday, April 7th 2014 from 10pm to 11pm (GMT+2)
Tokyo : Monday, April 7th 2014 from 11pm to 12am (GMT+2)
Sydney : Tuesday, April 8th 2014 from 01am to 02am (GMT+2)
Wellington : Tuesday, April 8th 2014 from 03am to 04am (GMT+2)
San Francisco : Monday, April 7th 2014 from 07am to 08am (GMT+2)
New York : Monday, April 7th 2014 from 10am to 11am (GMT+2)
Buenos Aires : Monday, April 7th 2014 from 11am to 12pm (GMT+2)
Reykjavik : Monday, April 7th 2014 from 02pm to 03pm (GMT+2)
London / Dublin : Monday, April 7th 2014 from 03pm to 04pm (GMT+2)
Paris / Berlin : Monday, April 7th 2014 from 04pm to 05pm (GMT+2)
Istanbul : Monday, April 7th 2014 from 05pm to 06pm (GMT+2)
Moscou / Dubaï : Monday, April 7th 2014 from 06pm to 07pm (GMT+2)
Bangkok : Monday, April 7th 2014 from 09pm to 10pm (GMT+2)
Shanghai : Monday, April 7th 2014 from 10pm to 11pm (GMT+2)
Tokyo : Monday, April 7th 2014 from 11pm to 12am (GMT+2)
Sydney : Tuesday, April 8th 2014 from 01am to 02am (GMT+2)
Wellington : Tuesday, April 8th 2014 from 03am to 04am (GMT+2)
New developments in BTK management. Endovascular management of Complex BTK arterial lesions
Live session from Charing Cross Symposium - London, UK
Share
May 2012
Honolulu : Wednesday, May 9th 2012 from 04am to 06:20am (GMT+2)
San Francisco : Wednesday, May 9th 2012 from 07am to 09:20am (GMT+2)
New York : Wednesday, May 9th 2012 from 10am to 12:20pm (GMT+2)
Buenos Aires : Wednesday, May 9th 2012 from 11am to 01:20pm (GMT+2)
Reykjavik : Wednesday, May 9th 2012 from 02pm to 04:20pm (GMT+2)
London / Dublin : Wednesday, May 9th 2012 from 03pm to 05:20pm (GMT+2)
Paris / Berlin : Wednesday, May 9th 2012 from 04pm to 06:20pm (GMT+2)
Istanbul : Wednesday, May 9th 2012 from 05pm to 07:20pm (GMT+2)
Moscou / Dubaï : Wednesday, May 9th 2012 from 06pm to 08:20pm (GMT+2)
Bangkok : Wednesday, May 9th 2012 from 09pm to 11:20pm (GMT+2)
Shanghai : Wednesday, May 9th 2012 from 10pm to 12:20am (GMT+2)
Tokyo : Wednesday, May 9th 2012 from 11pm to 01:20am (GMT+2)
Sydney : Thursday, May 10th 2012 from 01am to 03:20am (GMT+2)
Wellington : Thursday, May 10th 2012 from 03am to 05:20am (GMT+2)
San Francisco : Wednesday, May 9th 2012 from 07am to 09:20am (GMT+2)
New York : Wednesday, May 9th 2012 from 10am to 12:20pm (GMT+2)
Buenos Aires : Wednesday, May 9th 2012 from 11am to 01:20pm (GMT+2)
Reykjavik : Wednesday, May 9th 2012 from 02pm to 04:20pm (GMT+2)
London / Dublin : Wednesday, May 9th 2012 from 03pm to 05:20pm (GMT+2)
Paris / Berlin : Wednesday, May 9th 2012 from 04pm to 06:20pm (GMT+2)
Istanbul : Wednesday, May 9th 2012 from 05pm to 07:20pm (GMT+2)
Moscou / Dubaï : Wednesday, May 9th 2012 from 06pm to 08:20pm (GMT+2)
Bangkok : Wednesday, May 9th 2012 from 09pm to 11:20pm (GMT+2)
Shanghai : Wednesday, May 9th 2012 from 10pm to 12:20am (GMT+2)
Tokyo : Wednesday, May 9th 2012 from 11pm to 01:20am (GMT+2)
Sydney : Thursday, May 10th 2012 from 01am to 03:20am (GMT+2)
Wellington : Thursday, May 10th 2012 from 03am to 05:20am (GMT+2)
Abbott Vascular Knowledge Center Education Program: CLI complex case management Live cases
from Abano Terme with Dr. Marco Manzi -
Share
Attempt of recanalization with previous surgical thrombectomy
Dr Hartung & Dr Neglen - Decision of non-intervention after diagnostic
Share
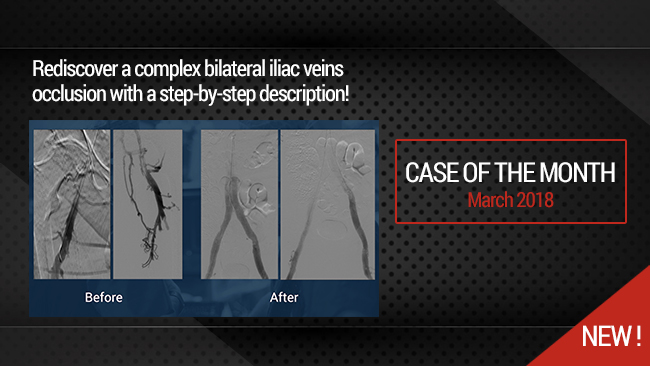
Post thrombotic syndrome with high grade compression stenosis of left iliac vein
Venous stenting. Live case from Arnsberg, Germany.
Share
BTK arteries angioplasty: Optimal Complex recanalization for BTK arteries (Drug Coated Balloon angio...
Case of the month: March 2019
Share











Sharif Khashaba K. kindly improve the voice
Vanessa R. How do you treat venous non thrombotic in stent restenosis
Gustavo R. In chronic oclusion how often did you see instent stenosis in Iliocaval Wallstent
Olivier H. in our experience on 162 patients with a median follow-up of 44 months, primary patency is 70% at 60 months and assisted primary patency 85%
Peter N. Using the Wallstent, the cumulative in-stent stenosis rate at 6 years is in non-thrombotic obstructions (NIVL) 1% and in postthrombotic obstructions approximately 10%. In-stent stenosis is then defined as being >50% lumen reduction. It is common to see some in-stent layering of
Jacobo N. What do you think is the best aproach to the lesion, popliteal or contralateral? Thanks
Olivier H. for chronic lesion, i prefer anterograde approach through the femoral or popliteal. Some teams favor internal jugular approach (must always be ready in case of IVC lesions)
for acute lesions, it depends on the patency of the popliteal vein. If occluded, jugular or controlateral acess
Maria Fabrizia G. do you use the same strategy in presence of PE?
Olivier H. PE does not change the strategy but can make discuss the use of an IVC filter
bander A. what is he indications in case of non thrombotic iliac vein lesion ?
Olivier H. symptomatic and disabled patients C2-6, pelvic congestion syndrome
Peter N. I agree with Olivier, but wants to qualify it slightly. As we pointed out in the discussion, compression of the iliac veins are common in the asymptomatic population and possibly up to 30% have >50% stenosis with no symptoms! So there is a potential risk of overtreatment. In chronic venous disease of the lower limb, treatment of the outflow obstruction is indicated in patients with the C-class in CEAP being marked swelling (C3) and those with skin changes/ulcers (C4-C6). In addition, you have those patients with venous pain without skin changes or varicose veins, which can not be solely explained by the presence of reflux, if any. We use visual analogue scale (VAS) to evaluate that, considering VAS >5 being significant. As Olivier pointed out the symptoms have to affect the patients' quality of life.
Sandeep S. When using three stents, why is the middle stent placed last in iliofemoral venous intervention?
Is there any algorithim to decide on when and not to stent across deep femoral vein?